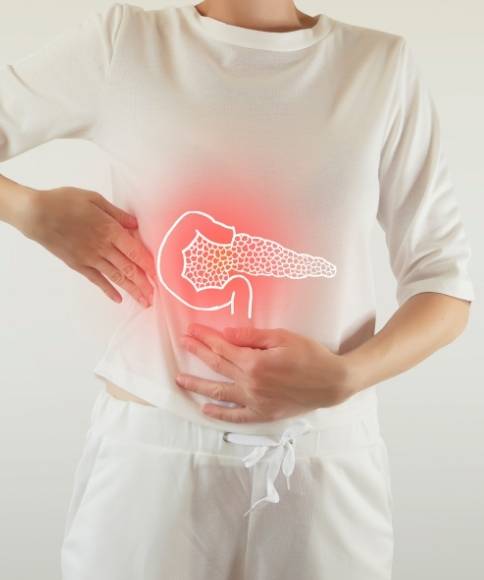
Pancreatitis develops within the pancreas which exists as a soft spongy leaf-shaped organ in the upper left stomach area near the posterior stomach location. This organ consists of three parts (head, body, then tail) lying among the small intestine, spleen and liver. The pancreas regulates blood sugar and aids digestion by producing enzymes. When pancreatitis triggers pancreatic inflammation, it increases the risk of developing pancreatic cancer if left untreated. An acute pancreatitis CT scan serves to diagnose this condition yet pancreatitis treatment requires either medication or dietary adjustments and surgical intervention for severe cases. The pancreas maintains blood supply through essential blood vessels including the superior mesenteric artery which together with the portal vein extends to provide circulation for the vital organ and adjacent tissues.
Disease of the pancreas
Pancreatitis
Pancreatitis is inflammation of the pancreas that occurs when pancreatic enzyme secretions build up and begin to digest the organ itself. It can occur as acute painful attacks lasting a matter of days, or it may be a chronic condition that progresses over a period of years. To learn more about pancreatitis, its causes, symptoms, and treatment options you can visit our Gastroenterology Services page for expert medical insights.
Acute pancreatitis
Acute pancreatitis refers to symptoms (usually abdominal pain) that develops suddenly, most often as a result of gallstones or alcohol ingestion. In rare circumstances, certain medications, trauma, and infectious causes can also lead to acute pancreatitis. Acute pancreatitis can be life threatening, but most patients recover completely.
Causes of acute pancreatitis
Acute pancreatitis is most commonly caused by gallstones or heavy alcohol consumption. Other causes include trauma, injury or surgery , ingestion of certain drugs (steroids, azathioprine and etc), lipid disorder and infection. Up to 15% of patients the cause of acute pancreatitis is unknown.
Symptoms of Acute Pancreatitis
- Severe, steady pain in the upper-middle part of the abdomen, often radiating into the back
- Jaundice
- Low-grade fever
- Nausea or vomiting
- Lowered blood pressure
- Clammy skin
- Unusual abdominal hardness or mass that can be felt
- Abdominal bloating and tenderness
- Bruising (ecchymosis) in the flanks and midsection
- The tissue of the pancreas may become necrotic (tissue death)
- Pancreatic abscess
- Pancreatic pseudocyst, which is an abnormal deposit of tissue, fluid and debris that can result after episodes of acute pancreatitis, typically 1 to 4 weeks after onset
Treatment of acute pancreatitis
Treatment of acute pancreatitis is mainly supportive. This include pain control and intravenous (IV) fluids, antibiotic and sometime nutrition. Surgery is rarely required for treatment of complication from acute pancreatitis.
Chronic pancreatitis
Chronic pancreatitis refers to continuous process in which the pancreas continues to sustain damage and lose function over time. The majority of cases of chronic pancreatitis result from ongoing alcohol abuse and smoking, but some cases are hereditary or genetic mutations.
Causes of Chronic Pancreatitis and Associated Risks
Excessive alcohol consumption throughout many years typically triggers chronic pancreatitis which results in pancreatic damage that creates scarring. Multiple factors other than alcohol abuse lead to pancreatitis development such as inherited conditions combined with gallstones or autoimmunity and elevated triglycerides in the body. Research indicates that genetic mutations might play a role in unidentified pancreatitis triggers but scientists have not identified the primary factors that lead to the condition. Chronic pancreatitis develops over time and increases pancreatic cancer risk, hence its CT findings differ from acute pancreatitis. Early detection and treatment of pancreatitis stabilize symptoms and prevent organ damage.
Symptoms of Chronic Pancreatitis
Symptoms may develop over a period of time without the sudden dramatic occurrence of an acute attack. There is a decrease in the secretion of enzymes needed for digestion and absorption of dietary fats, resulting in fatty stools. This is called exocrine insufficiency. Recurrent abdominal pain may be accompanied by nausea and weight loss. Diagnostic scans may find stones or areas of calcified tissue within the pancreas.
- Abdominal and/or back pain
- Weight loss
- Nausea and vomiting
- Onset of diabetes mellitus
- Pale colored, oily stools
Treatment of chronic pancreatitis
The basic treatment for chronic pancreatitis is nutritional support and pain management. Patients with exocrine insufficiency receive enzyme replacement treatment, and diabetics need endocrinologists. When pancreatitis is severe, surgery may be needed. Acute pancreatitis CT imaging and other tests are needed to diagnose and treat the illness, which can be caused by gallstones and alcohol. Patients with pancreatitis must follow dietary restrictions while managing pain and other concerns that increase pancreatic cancer risk.
If you need a specialist consultation for pancreatitis treatment or any other pancreatic condition, visit us at Mount Elizabeth Hospital for expert diagnosis and high quality medical care.